Section 1115’s demonstration waivers provide states with a means to test new approaches to Medicaid and generally reflect changing priorities from presidential administration to presidential administration. The Biden administration will encourage states to propose waivers to expand coverage, reduce health disparities, and promote “whole person care,” including by addressing health-related social needs (HRSN). I encourage it. Both states and the federal government have identified addressing social determinants of health (SDOH) as a key priority for Medicaid. The government recently expanded how states can use their Section 1115 powers by approving waivers in four states (Arkansas, Arizona, Massachusetts, and Oregon) that include certain HRSN services for targeted populations. provided further insight into how it can be used to address the social needs of registrants. These HRSN efforts cover a small portion of the total Medicaid population and Medicaid spending. In all four approvals, CMS stated that approved HRSN services “promote coverage, access, and quality of health care, improve health outcomes, reduce health disparities, and improve long-term and lower costs relative to traditional medical care.” It is hoped that this will lead to the creation of highly effective substitutes or supplements.” service. ” This issue brief provides an overview of how exemptions have been used to address societal needs, including an overview of recent approvals.
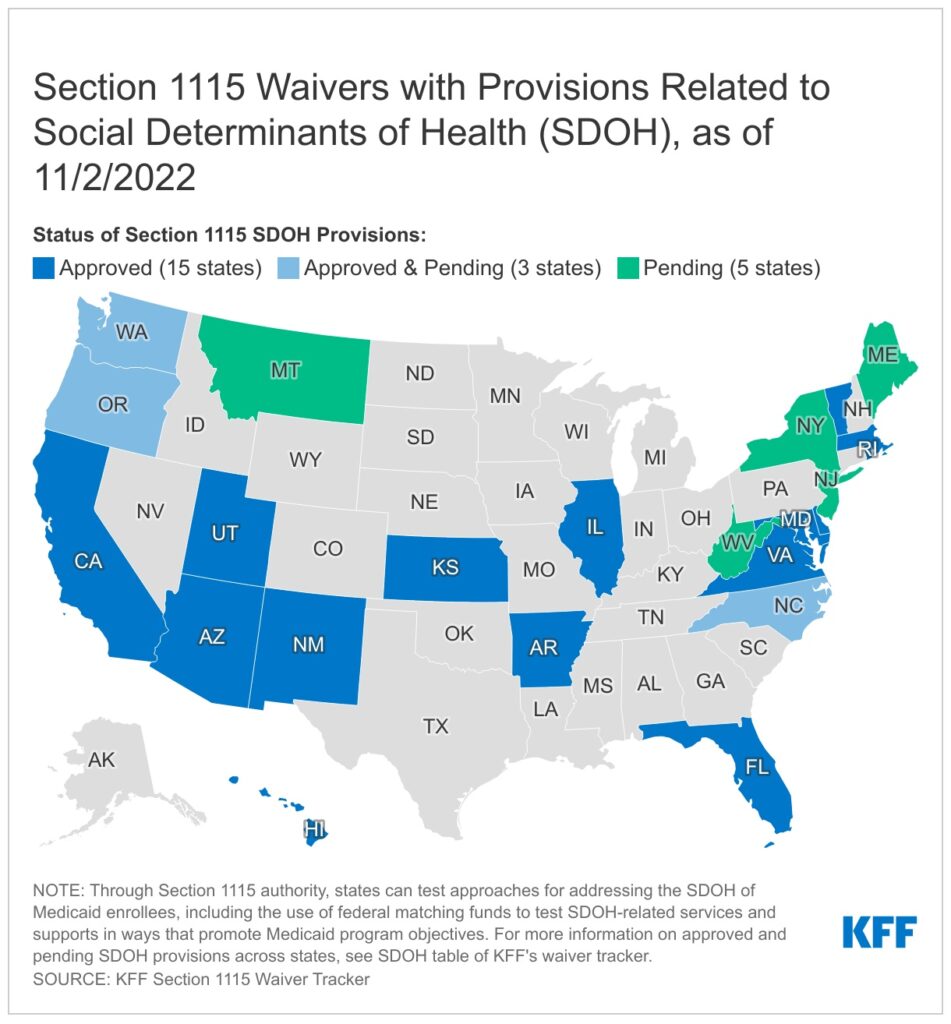
Many states utilize Section 1115 exemptions to address the social needs of Medicaid enrollees (Figure 1). SDOH is the conditions under which people are born, grow, live, work, and age that shape their health. These include, but are not limited to, housing, food, education, employment, healthy behaviors, transportation, and personal safety. Outside of Medicaid’s home and community-based services (HCBS) mandate, states have limited ability to use federal Medicaid funds to pay for the direct costs of non-medical services such as housing and food. However, in addition to state plans and managed care options, states can request Section 1115, which waives the authority to add certain non-clinical services to Medicaid benefit packages. As of November 2, 2022, 18 states have approved section 1115 waivers that include SDOH-related provisions, and 8 states have pending SDOH requests. The scope of services provided and the people covered by these exemptions vary and are very narrow in some states. It may also overlap with the HCBS program in some cases. Notable SDOH Section 1115 provisions approved before 2022 include:
- in north carolina The Healthy Opportunities pilot will target a limited number of skilled managed care enrollees who meet health and social risk factors to address housing instability, transportation safety, interpersonal violence, and toxic stress . The “Network Lead” will manage the network of human services organizations providing pilot services.
- Washington’s Accountable Communities of Health (ACH) is a lead organization that coordinates community projects designed to improve care for Medicaid enrollees. CMS approved funding for ACH-related performance incentives based on the premise that social health, public health, and community-based organizations play a role in the clinical delivery system.
- california The CalAIM initiative aims to implement the state’s whole-person care approach across the state. Under CalAIM, managed care plans provide enhanced care management and community support, also known as “in lieu of services” (ILOS), to high-need beneficiaries. Community supports include restorative care and posthospitalization short-term residential services (authorized under section 1115) and other ILOS authorized under the 1915b exemption.
In addition to these and recent approvals, eight states have requested CMS review of their pending SDOH regulations. For example, New York State recently called for an amendment to health equity reform that would establish community organizations to coordinate health equity efforts and provide evidence-based interventions to address social care needs. did. The request includes a menu of transitional housing and respite services for enrollees with specific high needs.
Fall 2022, CMS approved Exemptions from Article 1115 AR, arizona, Maand or It authorizes evidence-based HRSN services to address food insecurity and housing instability among identified high-need populations (Table 1). Who is eligible for HRSN services varies by state, but in each case it is a narrowly defined group that must meet specific health and social risk criteria. These groups represent a small percentage of each state’s overall Medicaid population (the exact number of enrollees covered by his HRSN initiative in each state will be determined in the state’s upcoming monitoring and evaluation report. Learn more (see paragraph below). Her HRSN services allowed also vary by state and may include housing assistance (such as short-term rent/transitional housing after transition). Nutritional support. and case management, outreach, and education. CMS approval emphasizes that licensed HRSN services must be clinically appropriate. That is, to receive HRSN services, enrollees must have a documented medical need for the services and the services must be medically appropriate based on clinical and social risk factors. must be judged.
In all four states, CMS approved spending authority for HRSN services and infrastructure, which required states to monitor and evaluate the impact of these services on program costs. Although not set forth in statute or regulation, a long-standing element of Section 1115’s waiver policy is that the waiver must be budget neutral to the federal government (i.e., federal costs under the waiver must be the amount that would have accrued in the state in the absence of the tax). The calculation of budget neutrality is complex and reflects a combination of per capita and total spending. For recent AR, AZ, MA, and OR approvals, CMS conducts annual filings. totalling Budget neutrality spending caps cap the HRSN service spending to which each state can receive federal financial participation (Table 2). These limits indicate that HRSN spending is a small portion of total exempt and Medicaid spending. For the fifth year of each demonstration, in Arkansas, Arizona, the cap on HRSN service spending is less than 1% of total Medicaid spending (FY 2021). , MA, and OR approximately 2% of total expenditures. In addition to the service itself, CMS also approved a small amount of funding for infrastructure investments to support the implementation and delivery of her HRSN services in all four states. Separate aggregate limits apply to this fund. Additionally, in order to maintain and/or improve enrollees’ access to quality care, each state must increase base Medicaid payments to at least 80% of Medicare, subject to approval by HRSN spending authorities in Arizona, Massachusetts, and Oregon. required to maintain the rate. Fees for primary care, behavioral health, and obstetric providers (fees below this level must increase). CMS notes that “research shows that increasing Medicaid payments to health care providers improves beneficiaries’ access to health care services and the quality of care they receive.”
In addition to HRSN services, CMS has approved continued eligibility provisions for MA and OR and continues to work with these states and other states on pre-release requests. States can choose a state plan option that provides 12 months of continued eligibility (CE) for Medicaid children, but not for other populations. Recent operating room exemption approvals included CE for children up to 6 years of age and her 2 year CE for children. all MA approval included a 12-month CE for enrollees released from a correctional facility and a 24-month CE for enrollees experiencing homelessness. CMS also recently approved her 12-month CE for eligible parents and other caring relatives in Kansas. States with pending CE requests include WA and NM (where state-level public comment was recently completed), both of which are pursuing CE for her children up to age 6, as well as OR. . Another Section 1115 issue to note in relation to eligibility is pre-release services. Eleven states (including Arizona, Massachusetts, and Oregon) require waivers from Medicaid inmate exclusion policies to provide pre-release coverage to certain inmates. Although CMS has not approved (or denied) any of these requests, the agency is writing to Arizona, Massachusetts, and Oregon to “increase pre-release services for law enforcement personnel and increase the number of individuals leaving facilities.” We support supporting their return.” in our communities and continue to work with the state on this part of the proposal.”
In the future, the results of the evaluations needed for HRSN efforts may inform future policy decisions about whether and how to use Medicaid to address the social needs of enrollees. there is. Section 1115 exemptions are subject to enhanced monitoring and evaluation requirements under the ACA. States must have a publicly available CMS-approved evaluation strategy that includes metrics related to coverage, access, and other outcomes. For example, states must regularly collect and report data that answers questions about the number of enrollees covered by the HRSN initiative. Prevalence and severity of social needs of enrollees. Enrollees receive preventive and routine care, as well as potentially avoidable emergency medical care. Cost-effectiveness of HRSN initiatives. States must also assess the impact of their efforts on overall access, quality, and health outcomes, as well as disparities in these outcomes. Evaluation requirements include a schedule of deliverables, including quarterly and annual monitoring reports, and interim and final evaluation reports. The results of these ongoing evaluations will inform operational challenges and determine the costs associated with these waivers and how effective the waivers are in addressing the health-related social needs of Medicaid enrollees. may help provide early insight.